Melioidosis: Perbedaan antara revisi
Hanamanteo (bicara | kontrib) baru Tag: halaman dengan galat kutipan |
Hanamanteo (bicara | kontrib) + Tag: halaman dengan galat kutipan |
||
| Baris 25: | Baris 25: | ||
| deaths = 89,000 people per year<ref name="Joost 2018"/> |
| deaths = 89,000 people per year<ref name="Joost 2018"/> |
||
}} |
}} |
||
'''Melioidosis''' adalah penyakit [[infeksi]] yang disebabkan oleh [[ |
'''Melioidosis''' adalah penyakit [[infeksi]] yang disebabkan oleh [[bakteri]] [[Gram-negatif]] bernama ''[[Burkholderia pseudomallei]]''.<ref name="Joost 2018"/> Kebanyakan orang yang dijangkiti ''Burkholderia pseudomallei'' tidak mengalami satupun gejala, tetapi mereka yang mengalami gejala memiliki tanda dan gejala seperti [[demam]], perubahan kulit, [[radang paru-paru]], dan [[bisul]], hingga [[ensefalomielitis|radang otak]], [[radang sendi]], dan [[kejang septik|tekanan darah rendah yang berbahaya]] yang menyebabkan kematian.<ref name="Joost 2018"/> About 10% of people with melioidosis develop symptoms that last longer than two months, termed "chronic melioidosis".<ref name="Joost 2018"/> |
||
Humans are infected with ''B. pseudomallei'' by contact with polluted water. The bacteria enter the body through wounds, inhalation, or ingestion. Person-to-person or animal-to-human transmission is extremely rare.<ref name="Joost 2018"/> The infection is [[Endemic (epidemiology)|constantly present]] in Southeast Asia, particularly in northeast [[Thailand]] and northern Australia.<ref name="Joost 2018"/> In developed countries, such as in Europe and the United States, cases of melioidosis are generally imported from countries where melioidosis is more common.<ref name="Currie 2015"/> The signs and symptoms of melioidosis resemble [[tuberculosis]] and misdiagnosis is common.<ref>{{Cite journal|last1=Brightman|first1=Christopher|last2=Locum|date=2020|title=Melioidosis: the Vietnamese time bomb|journal=Trends in Urology & Men's Health|language=en|volume=11|issue=3|pages=30–32|doi=10.1002/tre.753|issn=2044-3749|doi-access=free}}</ref><ref name="Yi 2014"/> Diagnosis is usually confirmed by the growth of ''B. pseudomallei'' from an infected person's blood or other bodily fluid.<ref name="Joost 2018"/> Those with melioidosis are treated first with an "intensive phase" course of intravenous antibiotics (most commonly [[ceftazidime]]) followed by a several-month treatment course of [[co-trimoxazole]].<ref name="Joost 2018"/> Even if properly treated, around 10% of people with melioidosis die from it. If improperly treated, the death rate could reach 40%.<ref name="Joost 2018"/> |
Humans are infected with ''B. pseudomallei'' by contact with polluted water. The bacteria enter the body through wounds, inhalation, or ingestion. Person-to-person or animal-to-human transmission is extremely rare.<ref name="Joost 2018"/> The infection is [[Endemic (epidemiology)|constantly present]] in Southeast Asia, particularly in northeast [[Thailand]] and northern Australia.<ref name="Joost 2018"/> In developed countries, such as in Europe and the United States, cases of melioidosis are generally imported from countries where melioidosis is more common.<ref name="Currie 2015"/> The signs and symptoms of melioidosis resemble [[tuberculosis]] and misdiagnosis is common.<ref>{{Cite journal|last1=Brightman|first1=Christopher|last2=Locum|date=2020|title=Melioidosis: the Vietnamese time bomb|journal=Trends in Urology & Men's Health|language=en|volume=11|issue=3|pages=30–32|doi=10.1002/tre.753|issn=2044-3749|doi-access=free}}</ref><ref name="Yi 2014"/> Diagnosis is usually confirmed by the growth of ''B. pseudomallei'' from an infected person's blood or other bodily fluid.<ref name="Joost 2018"/> Those with melioidosis are treated first with an "intensive phase" course of intravenous antibiotics (most commonly [[ceftazidime]]) followed by a several-month treatment course of [[co-trimoxazole]].<ref name="Joost 2018"/> Even if properly treated, around 10% of people with melioidosis die from it. If improperly treated, the death rate could reach 40%.<ref name="Joost 2018"/> |
||
Revisi per 28 Oktober 2021 18.00
Halaman ini sedang dipersiapkan dan dikembangkan sehingga mungkin terjadi perubahan besar. Anda dapat membantu dalam penyuntingan halaman ini. Halaman ini terakhir disunting oleh Hanamanteo (Kontrib • Log) 912 hari 1076 menit lalu. Jika Anda melihat halaman ini tidak disunting dalam beberapa hari, mohon hapus templat ini. |
| Melioidosis | |
|---|---|
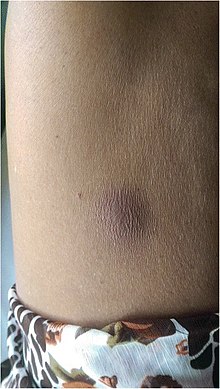 | |
| Bisul melioidosis di perut | |
| Informasi umum | |
| Spesialisasi | Penyakit menular |
| Penyebab | Burkholderia pseudomallei spread by contact to soil or water[1] |
| Faktor risiko | Diabetes mellitus, thalassaemia, alcoholism, chronic kidney disease[1] |
| Aspek klinis | |
| Gejala dan tanda | Tiada, demam, radang paru-paru, beberapa bisul[1] |
| Komplikasi | Encephalomyelitis, septic shock, acute pyelonephritis, septic arthritis, osteomyelitis[1] |
| Awal muncul | 1-21 hari setelah terjangkit[1] |
| Diagnosis | Growing the bacteria in culture mediums[1] |
| Kondisi serupa | Tuberculosis[2] |
| Tata laksana | |
| Pencegahan | Prevention from exposure to contaminated water, antibiotic prophylaxis[1] |
| Perawatan | Ceftazidime, meropenem, co-trimoxazole[1] |
| Distribusi dan frekuensi | |
| Prevalensi | 165,000 people per year[1] |
| Kematian | 89,000 people per year[1] |
Melioidosis adalah penyakit infeksi yang disebabkan oleh bakteri Gram-negatif bernama Burkholderia pseudomallei.[1] Kebanyakan orang yang dijangkiti Burkholderia pseudomallei tidak mengalami satupun gejala, tetapi mereka yang mengalami gejala memiliki tanda dan gejala seperti demam, perubahan kulit, radang paru-paru, dan bisul, hingga radang otak, radang sendi, dan tekanan darah rendah yang berbahaya yang menyebabkan kematian.[1] About 10% of people with melioidosis develop symptoms that last longer than two months, termed "chronic melioidosis".[1]
Humans are infected with B. pseudomallei by contact with polluted water. The bacteria enter the body through wounds, inhalation, or ingestion. Person-to-person or animal-to-human transmission is extremely rare.[1] The infection is constantly present in Southeast Asia, particularly in northeast Thailand and northern Australia.[1] In developed countries, such as in Europe and the United States, cases of melioidosis are generally imported from countries where melioidosis is more common.[3] The signs and symptoms of melioidosis resemble tuberculosis and misdiagnosis is common.[4][2] Diagnosis is usually confirmed by the growth of B. pseudomallei from an infected person's blood or other bodily fluid.[1] Those with melioidosis are treated first with an "intensive phase" course of intravenous antibiotics (most commonly ceftazidime) followed by a several-month treatment course of co-trimoxazole.[1] Even if properly treated, around 10% of people with melioidosis die from it. If improperly treated, the death rate could reach 40%.[1]
Efforts to prevent melioidosis include wearing protective gear while handling contaminated water, practising hand hygiene, drinking boiled water, and avoiding direct contact with soil, water, or heavy rain.[1] The antibiotic co-trimoxazole is used as a preventive only for individuals at high risk for getting melioidosis after being exposed to the bacteria.[1] No vaccine for melioidosis has been approved.[1]
Roughly 165,000 people are infected by melioidosis per year, resulting in about 89,000 deaths.[1] Diabetes is a major risk factor for melioidosis; over half of melioidosis cases are in people with diabetes.[1] Increased rainfall is associated with increased number of melioidosis cases in endemic areas.[2] It was first described by Alfred Whitmore in 1912 in present-day Myanmar.[5]
Referensi
- ^ a b c d e f g h i j k l m n o p q r s t u v w Kesalahan pengutipan: Tag
<ref>tidak sah; tidak ditemukan teks untuk ref bernamaJoost 2018 - ^ a b c Kesalahan pengutipan: Tag
<ref>tidak sah; tidak ditemukan teks untuk ref bernamaYi 2014 - ^ Kesalahan pengutipan: Tag
<ref>tidak sah; tidak ditemukan teks untuk ref bernamaCurrie 2015 - ^ Brightman, Christopher; Locum (2020). "Melioidosis: the Vietnamese time bomb". Trends in Urology & Men's Health (dalam bahasa Inggris). 11 (3): 30–32. doi:10.1002/tre.753
 . ISSN 2044-3749.
. ISSN 2044-3749.
- ^ Kesalahan pengutipan: Tag
<ref>tidak sah; tidak ditemukan teks untuk ref bernamaWhitmore 1912
Pranala luar
| Klasifikasi | |
|---|---|
| Sumber luar |
- Resource Center for melioidosis
- Templat:CDCDiseaseInfo
- Burkholderia pseudomallei genomes and related information at PATRIC, a Bioinformatics Resource Center funded by NIAID
- Monograph on Melioidosis (ISBN 978-0-444-53479-8); Elsevier Press, 2012, https://www.researchgate.net/publication/354857974_Monograph_Melioidosis-a-century-of-observation-and-research_ISBN_978-0-444-53479-8
